Why CAR T-Cell Therapy is the Last Resort for Blood Cancer
2025-10-28A diagnosis of a hematological malignancy, or blood cancer, is a life-changing event. These cancers affect all ages, but the picture looks different for children versus adults. Studies have shown that Leukemia is the most common childhood cancer, accounting for 25 percent of all cancer occurring before age 20.
While some blood cancers are highly prevalent in the young, the overall risk for many types—including most lymphomas and myelomas—increases significantly with age.
For decades, the foundation of treatment has been chemotherapy, radiation, and stem cell transplants. But for some patients, these cancers are particularly aggressive. They return, or "relapse," or they stop responding, becoming "refractory."
It is in this most difficult moment—when standard options are no longer working—that a powerful, modern therapy has emerged as a critical lifeline: CAR T-cell immunotherapy. At GHG, this therapy represents a new hope for patients with relapsed or refractory blood cancer. What is that? How effective can it be? Which hospital or institution can we trust? Keep scrolling, this blog might give you some hints.
What is Blood Cancer
Blood cancer is a group of cancers that affect the production and function of your blood cells. Most of these cancers start in your bone marrow, the body's "blood cell factory."
In a healthy person, stem cells in the bone marrow mature into red blood cells, white blood cells, and platelets.
In a person with blood cancer, this process is interrupted by the out-of-control growth of abnormal, cancerous cells. These abnormal cells crowd out the healthy ones, preventing your blood from doing its vital jobs, like fighting infections or preventing bleeding.
Types of Blood Cancers
While there are many variations, blood cancers are generally grouped into three main types:
- Leukemia: Found in the blood and bone marrow, this cancer is caused by the rapid production of abnormal white blood cells. These abnormal cells can't fight infection and impair the bone marrow's ability to make healthy red blood cells and platelets.
Read more:
CAR-T therapy for adult leukemia
- Lymphoma: This cancer affects the lymphatic system, a key part of your immune network. Abnormal white blood cells called lymphocytes become lymphoma cells, multiplying and collecting in your lymph nodes and other tissues, which compromises your immune system. GHG’s IIT programs target CD19 and CD20 markers in lymphomas
- Myeloma: This is a cancer of the plasma cells, a specific type of white blood cell in the bone marrow that produces antibodies to fight infection. The most common subtype is multiple myeloma. GHG has developed dual-target CAR-T therapies for multiple myeloma (BCMA/GPRC5D)
Other, rarer forms include Myeloproliferative Neoplasms (MPNs), where the bone marrow produces too many of a certain cell type, and Myelodysplastic Syndromes (MDS), where the bone marrow produces abnormal cells that don't mature or function properly. These rarer disorders are under investigation at GHG’s translational hematology cente
Symptoms of blood cancer
Common indicators of blood cancer are often related to this "crowding out" of healthy cells and can include:
- Persistent fatigue and weakness (from a lack of red blood cells, or anemia).
- Frequent or severe infections (from a lack of healthy white blood cells).
- Easy bruising or bleeding (from a lack of platelets).
- Other symptoms like drenching night sweats, unexplained weight loss, and swollen lymph nodes.
Traditional Blood Cancer Treatment Before CAR T-Cell Therapy
For decades, doctors have fought these cancers with a powerful arsenal of "traditional" treatments. The goal of this standard care is to destroy the cancerous cells and allow the bone marrow to resume its normal function.
|
Treatment |
How Does it Work |
|
Chemotherapy |
The most common treatment, which uses powerful drugs to kill fast-growing cancer cells. |
|
Radiotherapy |
Uses high-energy rays to damage the DNA of abnormal cells and stop them from replicating. |
|
Immunotherapy |
Uses the body's own immune system to fight cancer. This has traditionally included monoclonal antibodies, which are lab-made proteins that can mark cancer cells so the immune system can find and destroy them. |
|
Targeted Therapy |
Newer drugs that are designed to attack specific genetic mutations or proteins found on the cancer cells. |
|
Hematopoietic Stem Cell Transplantation (HSCT) |
Also known as a bone marrow transplant, this is an intensive procedure to replace the diseased bone marrow with healthy stem cells, either from the patient (autologous) or a donor (allogeneic). |
For many patients, these treatments are effective and can lead to long-term remission. But for some, the cancer is relentless. It either doesn't respond to these methods (refractory) or it returns after treatment (relapsed).
It was for these patients, who had run out of conventional options, that CAR T-cell therapy was developed. GHG’s clinical trials focus on this patient population
CAR T-Cell therapy for Blood Cancer
CAR T-cell therapy is a revolutionary form of T-cell immunotherapy that is fundamentally different from any other treatment.
How CAR T Works?
- Collection: A patient's T-cells (a type of immune cell) are collected from their blood in a process called leukapheresis.
- Re-engineering: These T-cells are sent to a highly specialized lab. There, they are genetically modified by introducing a "Chimeric Antigen Receptor," or CAR. This new receptor acts like a guided missile, training the T-cell to recognize and lock onto a specific protein (an antigen) on the surface of the cancer cells.
- Multiplication: These newly empowered "CAR T-cells" are multiplied in the lab, growing into an army of millions of cancer-fighting cells.
- Infusion: Before the infusion, the patient receives a short course of chemotherapy (called lymphodepletion) to "make room" for the new cells. The CAR T-cell army is then infused back into the patient's bloodstream, where they can begin their mission: to hunt and destroy any cell that carries their target antigen.
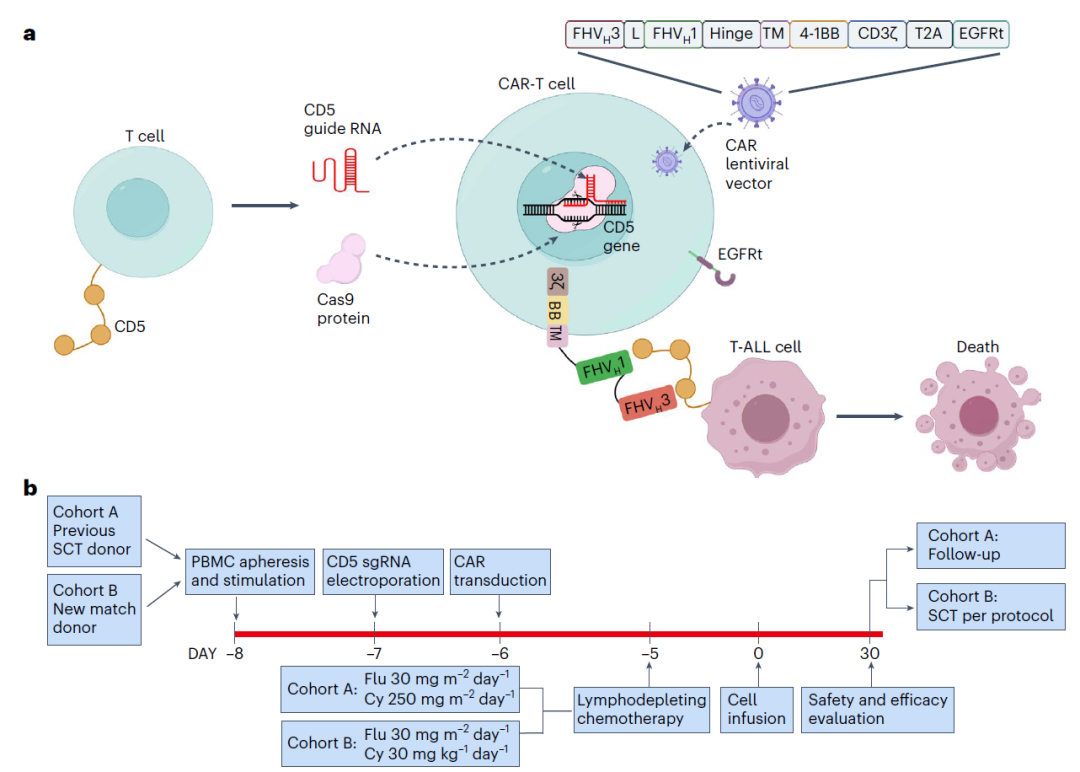
Copyright image from Allogeneic CD5-specific CAR-T therapy for relapsed/refractory T-ALL: a phase 1 trial
Commercial CAR T-Cell Therapy
These are the FDA-approved, pharmaceutical-led therapies available on the market. They are the result of years of research and have been proven effective in large-scale clinical trials for specific types of relapsed or refractory (R/R) blood cancers.
- Pros: These treatments are standardized, validated, and produced under an extremely high-standard system for manufacturing and testing.
- Challenges: This rigorous process comes with significant challenges. The research, development, and manufacturing costs are exceptionally high, which means the price for a single treatment is also very high (often described as being in the "million-yuan level"). Additionally, the manufacturing process is often centralized, which can lead to a long "vein-to-vein" time (the time from cell collection to infusion).
Investigator-Initiated Trials (IITs) CAR T-Cell Therapy
This is the second, and often more agile, path. An IIT (also known as "research-type CAR-T") is a clinical study that is initiated and led by doctors and researchers at their own hospital.
The primary goal of an IIT is not to get a drug to market, but to explore the efficacy and mechanisms of brand-new therapies. This is where the next generation of treatments is born. This model offers distinct advantages:
- Faster Access: Research hospitals like GoBroad often have in-house cell preparation, which can dramatically reduce the long wait times seen in the commercial pathway.
- Broader Innovation: IITs are where scientists can test new ideas, such as developing CAR T-cells for different targets or creating multi-target CAR T-cells designed to prevent the cancer from relapsing.
- Increased Accessibility: Because the goal is research and not commercial profit, the cost structure is different, and the fees are relatively lower, making these cutting-edge treatments a viable option for more eligible patients.
Side Effects of CAR T-Cell Therapy
The powerful immune activation triggered by CAR T-cells can lead to unique and sometimes severe side effects.
Cytokine Release Syndrome (CRS)
A widespread inflammatory response is caused by CAR T-cells activating and releasing a flood of chemicals called cytokines. Symptoms can range from mild to severe and often include:
- Fever (often the first sign)
- Chills or shaking
- Fatigue, muscle or joint pain
- Nausea, vomiting, diarrhea, loss of appetite
- Fast or irregular heartbeat, low blood pressure
- Difficulty breathing, low oxygen levels
- Headache, dizziness
Neurotoxicity (ICANS / CRES):
Also known as Immune Effector Cell-Associated Neurotoxicity Syndrome (ICANS), this involves inflammation affecting the brain and nervous system. It often occurs alongside or after CRS. Symptoms include:
- Headaches
- Confusion, delirium, difficulty concentrating
- Difficulty speaking (aphasia), slurred words, stuttering
- Changes in handwriting
- Weakness, shakiness (tremors), loss of coordination
- Dizziness, difficulty staying awake
- Memory loss, hallucinations
- Seizures (in severe cases)
B-Cell Aplasia & Increased Infection Risk
CAR T-cells targeting antigens like CD19 also eliminate healthy B-cells, which make infection-fighting antibodies. This leads to low antibody levels (hypogammaglobulinemia) and increases infection risk. Key signs include:
- Frequent or severe infections (respiratory, sinus, etc.)
- Fevers that aren't explained by CRS
- Slow recovery from common illnesses
Prolonged Low Blood Counts (Cytopenias)
These can be caused by the preparatory chemotherapy or the CAR T-cell activity itself and may take weeks or months to recover.
- Neutropenia (low neutrophils): Makes you vulnerable to bacterial infections.
- Anemia (low red blood cells): Can cause fatigue, weakness, pale skin, shortness of breath, and dizziness.
- Thrombocytopenia (low platelets): Can lead to easy bruising, bleeding (like nosebleeds or bleeding gums), and tiny red spots under the skin (petechiae).
*Note: Severity can range from mild to life-threatening. Always report any new or worsening symptoms to your medical team immediately.)
A Last Resort That Offers New Hope: GoBroad Healthcare Group (GHG)
For patients seeking advanced options beyond standard commercial therapies, GoBroad Healthcare Group (GHG) stands out as an international, research-driven hospital.

While CAR T-cell therapy is often considered a "last resort," we aim to make it a source of renewed hope through its focus on cutting-edge research and patient-centered care. For years, we strive to provide:
Pioneering Investigator-Initiated Trials (IITs) with Proven Impact
GHG is a leader in developing and conducting Investigator-Initiated Trials (IITs). It translates directly into providing patients access to the next generation of CAR T-cell therapies, treatments exploring novel targets and strategies often years before they become commercially available.
GHG's commitment to innovation is demonstrated by numerous achievements presented at major international conferences like the American Society of Hematology (ASH) and the European Hematology Association (EHA), as well as publications in leading medical journals, including Blood and Nature Medicine.

Copyright image from Nature Medicine
Rapid, High-Quality Cell Manufacturing
Leveraging significant technical advantages and an emphasis on research, GHG's approach to cell preparation within its own facilities aims to reduce the lengthy waiting times often associated with commercial CAR T-cell products. This focus allows for potentially faster delivery of treatment to patients in need.
A Diverse Portfolio of Novel Targets
Resistance and relapse are major challenges. GHG directly addresses this through its extensive research portfolio, offering CAR T-cell therapies aimed at a wide array of targets.
This includes single-target options (like CD19, CD20, CD22, CD7, CD5, BCMA, GPRC5D, CLL1, and more) as well as innovative dual-target CAR T-cells (like CD19-22 or CD19-20 sequential CAR-T). This broad range covers numerous types of leukemia, lymphoma, and myeloma, providing more tailored options to combat treatment resistance.
Expertise in Managing Complex Care
CAR T-cell therapy requires highly specialized management. GHG has established a comprehensive diagnosis and treatment system focused on CAR T-cell therapy, covering evaluation, implementation, monitoring, and supportive care to ensure patient safety throughout the process.
At GHG, we tend to bridge the gap between groundbreaking research and compassionate patient care. Offering you a vital path forward when other options seem exhausted.
Reference
https://my.clevelandclinic.org/health/diseases/22883-blood-cancer
https://www.mayoclinic.org/diseases-conditions/leukemia/diagnosis-treatment/drc-20374378
https://www.cancer.org/cancer/managing-cancer/treatment-types/immunotherapy/car-t-cell.html














